This checklist was co-created by community experts with a research team. Its purpose is to guide the practice of data science in mental health research.

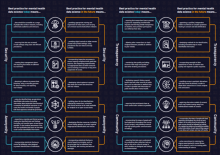
Click the links below to download the checklist:
![]() Booklet - Best Practice for Mental Health Data Science.pdf
Booklet - Best Practice for Mental Health Data Science.pdf
![]() A4 version - Best Practice for Mental Health Data Science.pdf
A4 version - Best Practice for Mental Health Data Science.pdf
Click here to access a text-only summary
How to use the checklist
The checklist is designed to complement other guidelines for data science practice, such as the UK Government’s
Data Ethics Framework. It gives researchers information about what is acceptable to, and important for, people
with lived experience of mental illness.
Researchers conducting new studies should consider each item on the today checklist and put measures
in place to meet these best practice criteria. Together as a research community, we should also aim to develop
and disseminate new protocols to meet the criteria for best practice in the future.
Case Studies
Data Science
Data science involves working with large data sets, containing information from many hundreds and thousands
of people – sometimes millions. These large data sets may be drawn from cohort studies, where participants
have chosen to enrol and given explicit permission for their data to be used. They may also deploy routine data –
information that is collected by health services for example, such as drug prescriptions or hospital admissions.
We can use these routine data to understand long-term trends in mental health, and – crucially – to capture
something of the experience of those people who don’t enrol in cohort studies or struggle to stay in touch.
Mental Health Data Science
Mental health data science involves those with experience of mental illness, or who may be at increased risk
of developing mental ill-health in the future. It is different from data science for physical conditions (such as cancer)
because of:
-
Stigma, which can still be associated with mental ill-health
-
The rich qualitative data available, such as routinely collected therapist case notes
-
Lack of trust/dissatisfaction with health services, that some people with mental ill-health express
Together, these factors may make people with mental illness feel less confident about data science, and more likely
to object to researchers accessing routine data without informed consent.
What can we do about this?
We believe it is essential to engage with stakeholders and use their perspectives to inform how mental health data
science is done.
To that end we recruited an expert task force of about 30 people who all had lived experience of mental illness and
professional knowledge about data science. Over three rounds, in early 2020, they helped us generate, refine and
then finalise this checklist which aims to define best practice in mental health data science from a well-informed,
lived experience perspective. The wording overleaf represents the distillation of their combined points of view.
The best practice checklist comes in two versions. The first version describes what researchers can do today
to ensure that their work is respectful and trustworthy. The second version describes what we, as a mental health
data science community, should deliver in the future for excellence in mental health data science.
To cite this checklist:
Kirkham, E.J., Iveson M., Beange, I., Crompton, C.J. Mcintosh, A. & Fletcher-Watson, S. (2020) A stakeholder-derived,
best practice checklist for mental health data science in the UK. University of Edinburgh.
Thank you
We would like to thank the Delphi experts who co-produced these guidelines, the MRC Pathfinder Stakeholder
Advisory Group at the University of Edinburgh, our MRC Pathfinder colleagues both within the University of Edinburgh
and across the UK, and all those who helped us to recruit our panel of experts.
